Damage Control in Penetrating Liver Trauma: Fear of the Unknown
Keywords:
REBOA, REBOVC, Penetrating Hemodynamically Unstable Liver Trauma., blood loss Surgical, hospital emergency service, algorithms, laparotomy, abdominal injuries, liverMain Article Content
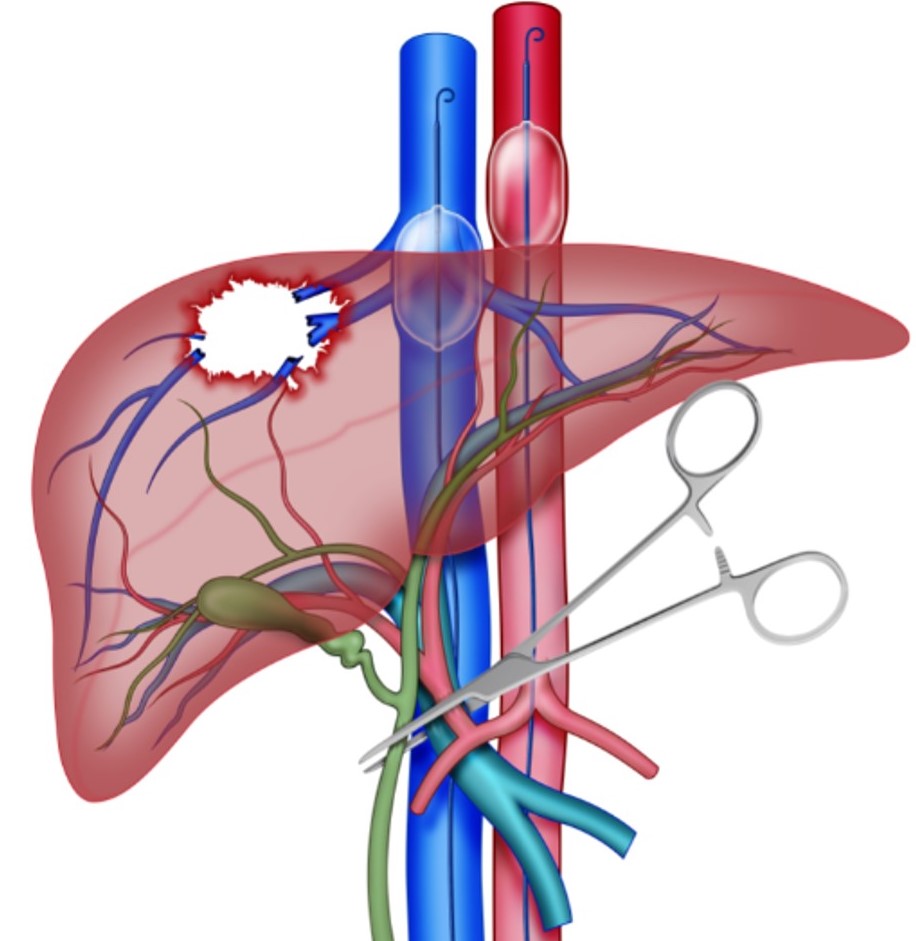
The liver is the most commonly affected solid organ in cases of abdominal trauma. Management of penetrating liver trauma is a challenge for surgeons but with the introduction of the concept of damage control surgery accompanied by significant technological advancements in radiologic imaging and endovascular techniques, the focus on treatment has changed significantly. The use of immediately accessible computed tomography as an integral tool for trauma evaluations for the precise staging of liver trauma has significantly increased the incidence of conservative non-operative management in hemodynamically stable trauma victims with liver injuries. However, complex liver injuries accompanied by hemodynamic instability are still associated with high mortality rates due to ongoing hemorrhage. The aim of this article is to perform an extensive review of the literature and to propose a management algorithm for hemodynamically unstable patients with penetrating liver injury, via an expert consensus. It is important to establish a multidisciplinary approach towards the management of patients with penetrating liver trauma and hemodynamic instability. The appropriate triage of these patients, the early activation of an institutional massive transfusion protocol, and the early control of hemorrhage are essential landmarks in lowering the overall mortality of these severely injured patients. To fear is to fear the unknown, and with the management algorithm proposed in this manuscript, we aim to shed light on the unknown regarding the management of the patient with a severely injured liver.
Downloads

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
The copy rights of the articles published in Colombia Médica belong to the Universidad del Valle. The contents of the articles that appear in the Journal are exclusively the responsibility of the authors and do not necessarily reflect the opinions of the Editorial Committee of the Journal. It is allowed to reproduce the material published in Colombia Médica without prior authorization for non-commercial use

 https://orcid.org/0000-0003-4495-7405
https://orcid.org/0000-0003-4495-7405