Abdominal actinomycosis by Actinomyces shaaliae georgiae mimicking neoplasia Case report
Keywords:
Actinomyces, Actinomycosis, Abdomen, Actinomycetaceae, Actinomyces georgiaeMain Article Content
Case Description:
We report the case of a 77-year-old male who presented with a three-week history of constitutional symptoms, accompanied by an indurated epigastric mass measuring 10 × 7 cm with a 4 cm phlyctenae, exhibiting local and systemic inflammatory responses.
Clinical Findings:
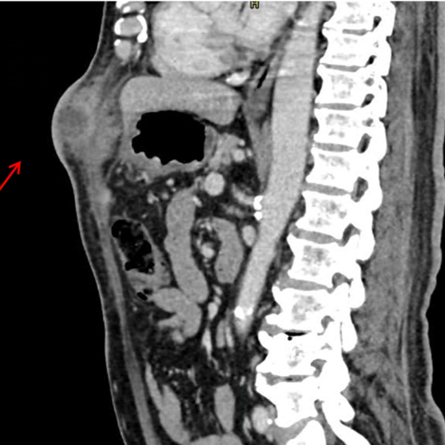
Abdominal computed tomography demonstrated focal thickening of the transverse colon with a poorly defined inflammatory lesion extending to the abdominal wall and a collection suggestive of colo-cutaneous fistula. The clinical and imaging findings raised a strong suspicion of malignancy. Microbiological culture from drainage material isolated Actinomyces shaaliae georgiae, further reinforcing the suspicion of neoplastic disease due to the tumor-like presentation.
Treatment and Outcomes:
Initial management included antimicrobial therapy and percutaneous drainage. Surgical exploration revealed a stony hard mass without cleavage planes, adherent to adjacent organs. Histopathological examination excluded malignancy, confirming an infectious process caused by A. shaaliae georgiae. The patient received prolonged antibiotic therapy, resulting in a favorable clinical outcome.
Clinical Relevance:
To our knowledge, this represents the first reported case of abdominal actinomycosis caused by A. shaaliae georgiae with this unique presentation. Actinomycotic lesions form purulent foci surrounded by extensive fibrosis, creating tumor-like masses that clinically and radiologically mimic neoplastic processes. This case expands the clinical spectrum and microbiological repertoire of A. shaaliae georgiae, emphasizing the critical importance of maintaining high clinical suspicion, implementing multidisciplinary diagnostic approaches, and ensuring appropriate antimicrobial management in abdominal actinomycosis to avoid unnecessary surgical interventions and improve patient outcomes.
Wong VK, Turmezei TD, Weston VC: Actinomycosis. BMJ. 2011, 343:6099. https://doi.org/10.1136/bmj.d6099 PMid:21990282 DOI: https://doi.org/10.1136/bmj.d6099
Valour F, Sénéchal A, Dupieux C, et al.: Actinomycosis: etiology, clinical features, diagnosis, treatment, and management. Infect Drug Resist. 2014, 7:183-97. https://doi.org/10.2147/IDR.S39601 PMid:25045274 PMCid:PMC4094581 DOI: https://doi.org/10.2147/IDR.S39601
Könönen E, Wade WG: Actinomyces and related organisms in human infections. Clin Microbiol Rev. 2015, 28:419-42. https://doi.org/10.1128/CMR.00100-14 PMid:25788515 PMCid:PMC4402957 DOI: https://doi.org/10.1128/CMR.00100-14
Lewis RP, Sutter VL, Finegold SM: Bone infections involving anaerobic bacteria. Medicine (Baltimore). 1978, 57:279-305. https://doi.org/10.1097/00005792-197807000-00001 PMid:207946 DOI: https://doi.org/10.1097/00005792-197807000-00001
Mabeza GF, Macfarlane J: Pulmonary actinomycosis. Eur Respir J. 2003, 21:545-51. https://doi.org/10.1183/09031936.03.00089103 PMid:12662015 DOI: https://doi.org/10.1183/09031936.03.00089103
Bennett JE, Dolin R, Blaser MJ. Mandell, Douglas, and Bennett's principles and practice of infectious diseases E-Book: 2-volume set. Elsevier health sciences, 2019.
Heo SH, Shin SS, Kim JW, et al.: Imaging of actinomycosis in various organs: a comprehensive review. Radiographics. 2014, 34:19-33. https://doi.org/10.1148/rg.341135077 PMid:24428279 DOI: https://doi.org/10.1148/rg.341135077
Triantopoulou C, der Molen AV, Es ACV, Giannila M: Abdominopelvic actinomycosis: spectrum of imaging findings and common mimickers. Acta Radiol Short Rep. 2014, 3:2047981614524570. https://doi.org/10.1177/2047981614524570 DOI: https://doi.org/10.1177/2047981614524570
PMid:24778807 PMCid:PMC4001438
Sung HY, Lee IS, Kim SI, et al.: Clinical Features of Abdominal Actinomycosis: A 15-year Experience of A Single Institute. J Korean Med Sci. 2011, 26:932-7. https://doi.org/10.3346/jkms.2011.26.7.932 PMid:21738348 PMCid:PMC3124725 DOI: https://doi.org/10.3346/jkms.2011.26.7.932
Rahimkhani M, Mordadi A, Kazemian K, Khalili H: Comparison of helicobacter pylori detection methods: It's association with leukocytosis and monocytosis. Infectious Disorders - Drug Targets. 2020, 20(6):920-924. https://doi.org/10.2174/1871526520666200707113955 PMid:32634084 DOI: https://doi.org/10.2174/1871526520666200707113955
Choi M-M, Baek JH, Lee JN, Park S, Lee W-S: Clinical features of abdominopelvic actinomycosis: report of twenty cases and literature review. Yonsei Med J. 2009, 50:555-9. https://doi.org/10.3349/ymj.2009.50.4.555 PMid:19718405 PMCid:PMC2730619 DOI: https://doi.org/10.3349/ymj.2009.50.4.555
Vasilescu AM, Târcoveanu E, Lupascu C, Blaj M, Lupascu Ursulescu C, Bradea C: Abdominopelvic Actinomycosis-The Diagnostic and Therapeutic Challenge of the Most Misdiagnosed Disease. Life. 2022, 12:447. https://doi.org/10.3390/life12030447 PMid:35330198 PMCid:PMC8954618 DOI: https://doi.org/10.3390/life12030447
Arslan RS, Koca YS, Beyoğlu R, Yenipazar AE: Appendecular actinomycosis: A case series of 14 patients. Med Clin (Barc). 2024, 162:500-4. https://doi.org/10.1016/j.medcli.2024.02.005 PMid:38570296 DOI: https://doi.org/10.1016/j.medcli.2024.02.005
Downloads

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
The copy rights of the articles published in Colombia Médica belong to the Universidad del Valle. The contents of the articles that appear in the Journal are exclusively the responsibility of the authors and do not necessarily reflect the opinions of the Editorial Committee of the Journal. It is allowed to reproduce the material published in Colombia Médica without prior authorization for non-commercial use

 https://orcid.org/0009-0001-8524-9512
https://orcid.org/0009-0001-8524-9512